Aesthetic Foot Surgery Podiatrist
Dr. Vladimir Zeetser, DPM, FACFAS
Premier Foot and Ankle Surgeon
5400 Balboa Boulevard, Suite 325
Encino, California 91316
For Appointment or Consultation:
| Telephone: | (818) 907-6100 |
| Email: | info@drzeetser.com |
Click here to request an appointment
With offices in Encino, CA, Aesthetic Foot Surgery Podiatrist Dr. Zeetser sees patients from all over Southern California for treatment of their foot and ankle problems.
Reconstructive Foot & Ankle Surgery by Podiatrist Dr. Vladimir Zeetser
Reconstructive Foot and Ankle surgery is aimed at correcting structural deformities, whether congenital or acquired, to restore function and eliminate or reduce pain. This is distinguished from aesthetic surgery, which is typically performed to correct deformities for cosmetic reasons that are not currently painful.
Dr. Zeetser performs all aspects of reconstructive foot and ankle surgery, ranging from minor to very complex. He treats patients of all ages, including children, adults and the elderly. He combines state of art implants and fixation devices with the latest and most innovative procedures available today.
The most common procedures he performs are:
- Bunion Correction
- Advanced Modified Mini-TightRope Bunion Surgery
- Hammertoe Correction
- Hallux Limitus/Rigidus (stiff big toe) Correction with or without implant arthroplasty
- Tailor's Bunion Correction
- Flatfoot Correction with or without implant
- Ball of the Foot Pain Correction (Metatarsal pain)
- Foot and Ankle Arthritis Repair
- Trauma Surgery for fractures, tendon and soft tissue tears
Additional Services Include:
- Aesthetic procedures
- Custom Orthotics, braces and splints
- Heel pain and Plantar Fasciitis treatment including surgery with non-invasive Extracorporeal Shockwave Therapy (ESWT)
- TOPAZ Procedure for Achilles tendon injuries and Plantar fasciitis
- Viscosupplementation with injections of synthetic joint fluid to treat arthritis
- Bone spurs
- Ingrown toenail surgical correction
- Neuroma treatment
- Plantar Wart treatment
- Platelet Rich Plasma (PRP) for tendon injuries
- Skin and Nail treatment for corns, calluses, rashes and infections, including fungal nails
- Sports Medicine for the treatment of ankle sprains, foot sprains and tendonitis
- Lower Extremity Swelling Control
- Varicose and spider veins
- Infrared Light Therapy (Anodyne) for Neuropathy and musculoskeletal pain
- Physical Therapy for the lower extremity
- Second opinions
- Wound care and Limb Salvage
Foot Feminization Surgery by Dr. Vladimir Zeetser
Dr. Zeetser is considered the premiere foot and ankle surgeon in the United States performing his renowned FootFem Foot Feminization Procedures for those individuals seeking a more feminine and beautiful foot and ankle.
His Aesthetic & Functional Foot Surgery provides patients with all areas of improvement, including:
- Aesthetic Toe Shortening or Lengthening
- Bunion Correction - FastForward Bunion Correction System
- Foot Narrowing Procedure
- Fat Pad Augmentation
- Foot Deformity Correction
- Corn & Callus Removal
- Nail Fungus & Ingrown Nail Correction
- Sclerotherapy for Varicose and Spider Veins
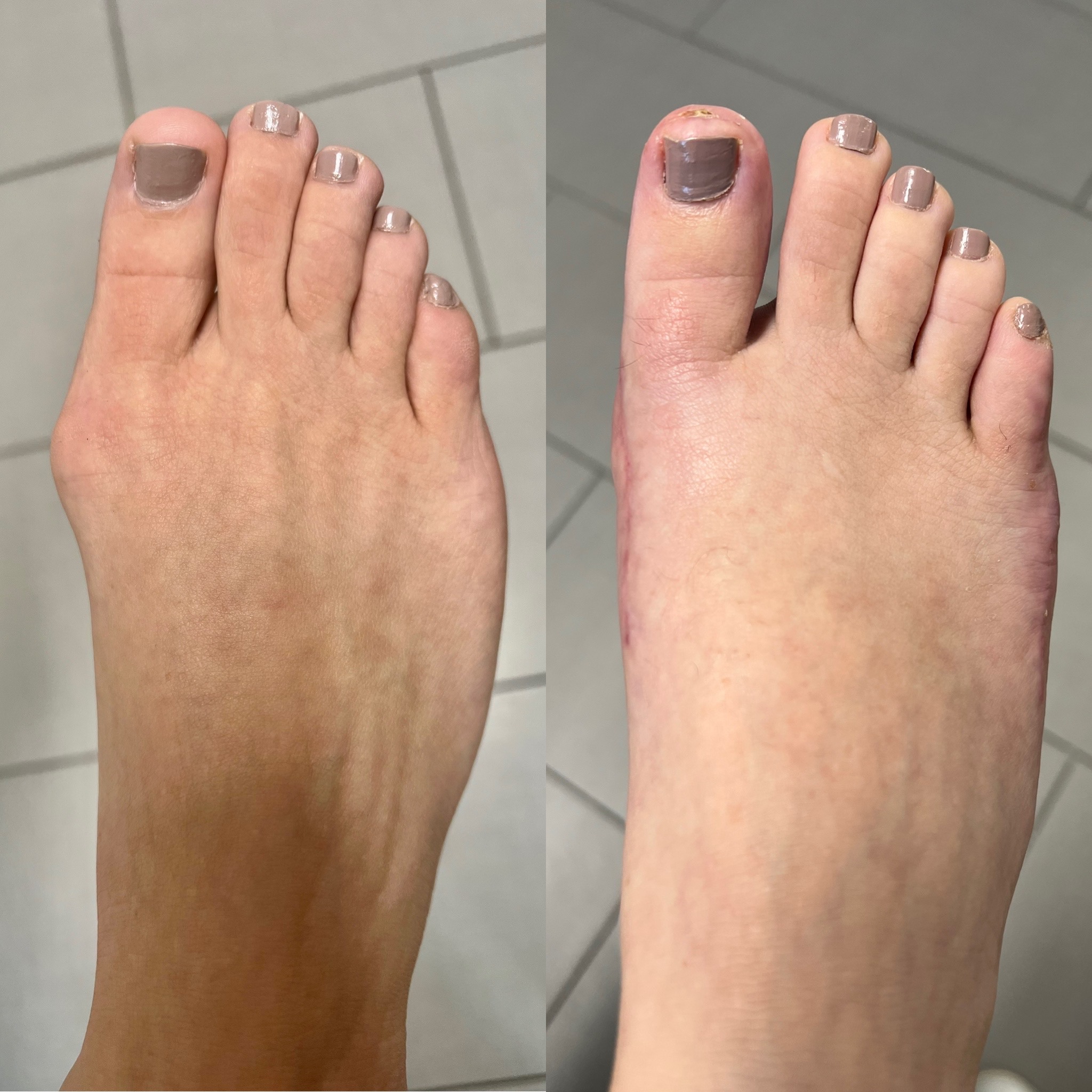
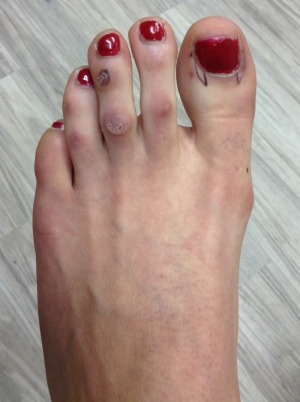
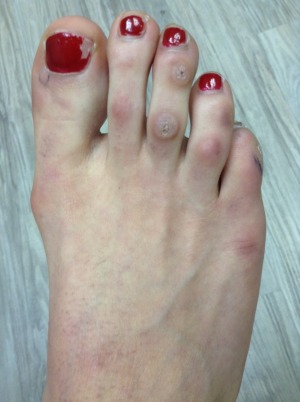
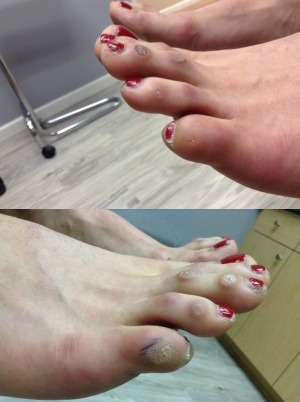
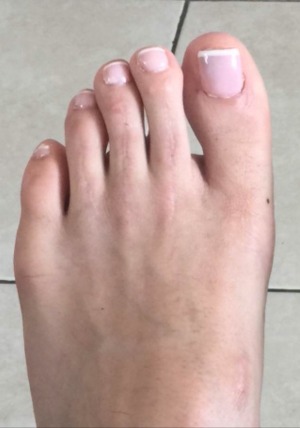
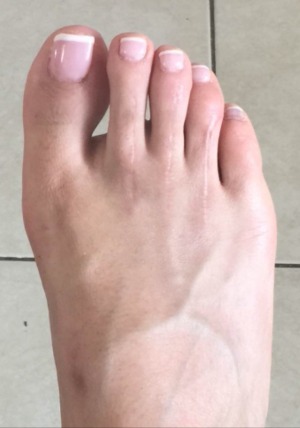
Before/After
Before
After
These procedures were performed by Dr. Vladimir Zeetser.
Advanced Modified Mini-TightRope Bunion Surgery
Dr. Zeetser is an expert in the field of Bunion Correction Repair Surgery, and utilizes several different techniques to achieve the perfect outcomes for his patients.
The treatment of hallux valgus deformity includes the assessment of the hallux valgus angle, the intermetatarsal angle and the contribution of an interphalageus deformity. Additionally, there must be an assessment of the presence or absence of arthritic involvement of both the first metatarsocuneiform joint and the first metatarsophalangeal joint. Other considerations are the orientation of the distal metatarsal articular angle and the orientation and stability of the first metatarsocuneiform joint.
Contact Dr. Zeetser today for a Bunion Correction consultation by calling 818-907-6100
Botox injections for excessive foot sweating
Excessive sweating (hyperhidrosis) of the plantar aspect of the feet is a common problem affected many people. Besides being an uncomfortable hygienic condition, contributing to fungal infection and Athlete's foot, it can be an equally embarrassing problem creating social and psychological concerns. Botox injections for the bottom of the feet is a relatively new concept, but conforms well to the general increased awareness for aesthetic and hygienic concerns affecting daily life. Previously used safely in the foot for the treatment of spastic muscular conditions, such as in the Achilles tendon for spastic Cerebral palsy, Botox (botulinum toxin type A) has been used by plastic and aesthetic physicians for many years. In 2004, the FDA approved Botox for the treatment of excessive sweating. When topical antiperspirants and other drying agents are ineffective, Botox has been used as a safe and effective method for the treatment of excessive sweating in the bottom of the feet. Its mechanism of action is to temporarily block the secretion of the chemical responsible for activating sweat glands and thus interrupts sweating at the area where is has been injected.
Dr. Zeetser can administer these injections in the office following a local anesthetic injection to numb the bottom of the foot. Many other physicians performing this procedure rely on topical creams or ice to numb the area, which is not sufficiently effective on the foot. The procedure is relatively quick and painless once anesthesia has been achieved. After the procedure, there is no significant restriction to activities. Mild temporary bruising and tenderness can occur. Nothing can completely cure hyperhidrosis and this procedure is designed to control the condition. Sweating may return gradually on average within 6 months. Further injections may be required to maintain the desired effect at intervals varying between 7-16 months, depending on the individual patient.
Diabetic Foot Wounds Treatment
There are over than 21 million known people with diabetes in the United States, and this staggering figure continues to grow by almost one-half million annually. It has been estimated that an equal number of persons with diabetes remain undiagnosed. A person develops diabetes when their body is unable to maintain a normal level of sugar in the blood. Insulin, the hormone that regulates the level of sugar, is either not used properly by the body or it is produced in inadequate amounts. When this occurs, diabetes is the result.
Diabetes wreaks havoc with many major organ systems in the human body. Among others, it tends to create some of the worst and life altering complications in the feet. Over one half of diabetic hospital admissions are foot related. This is typically due to the disease process' effect on the nerves and blood vessels. As a result, the main complications include neuropathy (altered sensations which can eventually lead to numbness), peripheral arterial disease, increased risk of infection, decrease in tissue integrity and compromised healing capacity.
Minimally Invasive Fat Injection Treatment for Foot Pad Tissue Augmentation
Foot pad atrophy, the thinning or loss of the natural fat padding under the feet, can cause
significant discomfort and pain, especially when standing or walking. As we age or due to
specific conditions, the natural cushioning in the foot deteriorates, leaving the bones and soft
tissues exposed to increased pressure and stress. This condition can make walking or even
standing for long periods unbearable, often leading to further issues such as calluses, blisters,
and joint pain.
Dr. Vladimir Zeetser utilizes novel and effective fat injections treatment with Leneva and
Sculptra, offering a minimally invasive solution to restore lost cushioning and relieve foot pain.
What Are Fat Injections?
Fat injections for foot pad augmentation involve the injection of a specialized fat-based or fat-
stimulating product into the bottom of the foot. These injections are designed to restore the
natural padding that has been lost over time, offering relief from pain and discomfort caused by
foot pad atrophy.
The two most commonly used options for foot pad augmentation that Dr. Zeetser uses are:
- Leneva: A human-derived allograft adipose matrix, Leneva is a form of fat tissue that
promotes the regeneration of your body's natural fat in the foot. When injected into
areas of the foot where fat has been lost, Leneva acts as a scaffold that encourages the
growth of new, healthy fat cells, which gradually rebuild the natural padding of the foot.
- Sculptra: While traditionally used as a facial filler, Sculptra is also used in foot pad
augmentation. This product is a poly-L-lactic acid (PLLA) solution that stimulates
collagen production, helping to thicken and rebuild the soft tissue in the feet over time.
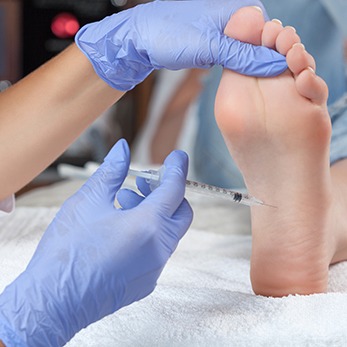 Key Benefits of Fat Injections for Foot Pad Augmentation
Key Benefits of Fat Injections for Foot Pad Augmentation
- Pain Relief and Improved Comfort The primary goal of fat injections is to alleviate pain
caused by the thinning of the foot's natural padding. By restoring this lost cushioning,
fat injections help to reduce the direct pressure on bones, nerves, and soft tissues,
resulting in immediate and long-term pain relief. This makes it easier to walk, stand, and
engage in daily activities without the constant discomfort that foot pad atrophy causes.
- Minimally Invasive Procedure Fat injections are a minimally invasive procedure
compared to surgical options. They are performed in an outpatient setting, usually with
a local anesthetic. The injections take only a short time to administer, and there is
minimal recovery involved. Most patients can return to their normal activities soon after
the procedure, making it a convenient solution for those seeking quick and effective
relief.
- Natural and Long-Lasting Results Treatments like Leneva and Sculptra encourage the
body's natural processes to restore lost tissue. Leneva works by regenerating fat cells in
the areas where it is injected, effectively rebuilding the natural foot padding. Sculptra
stimulates collagen production, which thickens the skin and soft tissues of the foot. Both
methods offer long-lasting results, and because they work with the body's natural
systems, the augmentation feels and functions like the original tissue.
- Customized Treatment Every patient's foot anatomy and condition are unique, which
means treatment needs to be tailored to each individual. Fat injections can be
customized to target the specific areas where cushioning is needed, allowing for a highly
personalized treatment plan. Whether you need padding in the ball of your foot, heel,
or both, fat injections can be adjusted to meet your specific needs.
- Reduced Risk of Complications Since fat injections are a non-surgical procedure and use
biocompatible materials, the risk of complications is minimal. There's no need for
incisions or implants, which means less risk of infection, scarring, or adverse reactions.
Both Leneva and Sculptra are safe, FDA-approved products, and patients typically
tolerate these treatments very well.
- Enhanced Mobility and Quality of Life Foot pad atrophy can severely limit mobility,
making it difficult to perform even basic tasks like walking or exercising. By restoring the
natural cushioning in the foot, fat injections improve mobility and allow patients to be
more active without pain. This enhanced mobility leads to a better quality of life, as
patients can participate in activities they may have avoided due to discomfort.
- Alternative to Surgery Many patients seek out fat injections as a less invasive
alternative to foot surgery. Surgical options for foot pad augmentation often involve
more extensive procedures with longer recovery times and a higher risk of
complications. Fat injections, on the other hand, offer a quicker, less invasive option
that can deliver significant relief without the need for surgery.
Who is a Good Candidate for Fat Injections?
Fat injections for foot pad augmentation are ideal for individuals who suffer from foot pad
atrophy and experience pain or discomfort when walking or standing. It is particularly beneficial
for patients who have tried other conservative treatments, such as orthotics or special shoes,
without achieving sufficient relief. Additionally, people who are looking for a minimally invasive
solution to avoid surgery may find fat injections to be a suitable option.
If you are experiencing pain and discomfort due to the loss of natural cushioning in your feet,
fat injections treatment offered by Dr. Zeetser offer a safe, effective, and minimally invasive
solution. These treatments restore the natural padding in your feet, helping to alleviate pain,
improve mobility, and enhance your overall quality of life. By using the body's natural processes
to regenerate lost tissue, fat injections provide long-lasting results that can help you get back
on your feet and enjoy life to the fullest.
Contact our office today for an appointment or consultation with Dr. Zeetser or call:
818-907-6100
For Appointment Or Consultation, Call
818-907-6100

Dr. Vladimir Zeetser is a board certified podiatric physician and surgeon specializing in reconstructive foot and ankle surgery. He is certified by the American Board of Podiatric Surgery both in Foot Surgery and Reconstructive Rearfoot and Ankle Surgery. His training includes advanced wound management and limb salvage and he has consistently achieved unparalleled results in healing problematic wounds. As an innovator and trendsetter in his field, he has been progressive in expanding aesthetic foot surgery and associated procedures to improve his patients' self-image while achieving among the highest functional outcomes and levels of patient satisfaction. Apparently unconventional in his practice approach, Dr. Zeetser believes that surgery should be minimally painful with a convenient and tolerable recovery, while producing the maximum results. He believes that the aesthetic result of any procedure is not a secondary consideration, but is just as important as the primary condition being corrected.
Dr. Zeetser treats all aspects of foot and ankle structural disorders, including lower extremity muscular, neurological, vascular and skin conditions. During your consultation, Dr. Zeetser always performs a thorough evaluation, explains his findings in detail and creates a treatment plan tailored to your specific needs. With all of your options presented in an understandable manner, you participate equally in the decision making for the treatment of your foot or ankle condition.
Disclaimer - The content on this site is for informational purposes only. You are encouraged to perform your own research into common foot problems and treatments available. It is not intended for the purpose of self-diagnosis or treatment recommendations. Only a personalized consultation can appropriately address your specific concern. - Dr. Zeetser